
We provide a unique blend of expertise, empathy, and advanced technology.
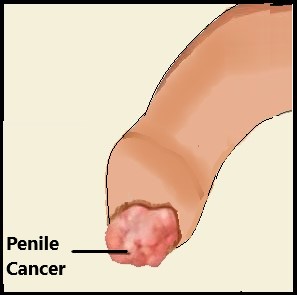
Here are some common questions about our Penile Cancer and how we can help you.
Common signs include lumps, changes in skin color, or unusual discharge. Early diagnosis is crucial for better outcomes.
Look for board-certified urologists specializing in penile cancer, check reviews, and consider asking for referrals.
Treatment may include surgery, radiation, chemotherapy, or immunotherapy; often customized to individual patient needs.
Yes, especially when caught early. Our specialists provide effective treatments to improve outcomes significantly.

Tailored strategies focusing on individual needs and circumstances.

Access to top specialists for comprehensive care and guidance.

Utilization of the latest techniques for effective and minimally invasive treatments.

Emotional and psychological assistance throughout the treatment journey.

Focus on overall well-being, integrating physical, mental, and emotional health in care.

Get treated at the First and Only Standalone NABH fully accredited Urology hospital in Gujarat.
It's natural to feel anxious about treatment. Our specialists ensure you have all the information.
We prioritize patient comfort. Pain management protocols are implemented to ensure a tolerable experience.
Costs vary depending on treatment plans. We provide detailed estimates and payment options during your consultation.
Our team is dedicated to creating a safe, understanding environment where you can express concerns without judgment.
Each treatment comes with its risks, but we thoroughly discuss these with you to ensure informed decisions.
Our pricing structure is transparent and competitive, ensuring patients receive premium care within their budget.
Detailed evaluation and discussion of symptoms.
Prices vary based on tests required.
Costs depend on the type of treatment selected.
I felt cared for every step of the way.
Hear from our patients about their experiences.